Radiation is a cancer treatment method that can shrink tumors or kill lingering cancer cells left behind by other treatment methods. It's also great for pain control. Radiation can extend your dog’s life and also improve quality of life.
Key Takeaways
- After radiation treatment, dogs can live anywhere from 9 months to over two years, this can vary widely depending on your dog’s exact case.
- Some dogs that receive treatment for pain relief alone may live for less, but for some tumors, radiation therapy can lead to 5 or more years of survival.
- You should give your dog radiation therapy if your veterinarian recommends it, and it is a realistic option for you and your dog.
- Radiation is a highly effective method of killing cancer cells. It has many applications for improving quality of life and extending survival time but it does not work for all cancers and is not a good fit for every dog or family.
- The side effects of radiation in dogs depend on the area of the body that the radiation beam goes through. Side effects can include skin irritation, tissue death, hair loss, color changes, and diarrhea. In very rare cases, radiation therapy can cause cancer in the treated area.
- Generally, radiation for dogs costs between $1200 and $8,000 for the total course.
- Radiotherapy is not painful for dogs, but side effects after treatment can cause temporary discomfort.
- Tumors can grow back after radiation depending on the tumor type, size, area, and intent of radiation protocol. The regrowth rate can range from months to over five years with no recurrence.
When Veterinarians Want to Use Radiation for Dogs
There are several methods and schedules for administering radiation for dogs, and the number of treatments and spacing between them depends on the machine type available, tumor type, location, and treatment goal.
If your dog is a candidate for radiation therapy, your veterinarian will discuss the details of your dog’s case with you, but radiation therapy is used in four primary situations:
- To treat remaining cancer that is not visible to our eyes (microscopic disease) after surgery.
- To shrink a tumor to make its removal easier.
- To treat tumors that can’t be removed surgically.
- To aid in pain control.
Radiation therapy can decrease the number of cancer cells in an area to improve quality of life by reducing pain. It can be used as a single therapy or in combination with other treatment methods depending on the cancer type, severity, location, and patient overall health.
How Radiation Works
Radiation therapy directly kills cancer cells by damaging their DNA.
It uses ionizing activity to do this. The linear accelerator produces ionizing radiation, and the beams pass through tissues and remove electrons from cells and molecules. This eventually damages those cells enough that they cannot divide and/or survive.
The killing of the cancer cells is not immediate because they typically do not die until they try to divide after treatment.
The machines that deliver this treatment aim a beam very specifically from different angles to target cancer while trying to avoid healthy tissue as much as possible. Only cells directly in the path of the beam are affected by the radiation.
Types of Radiation Therapy
There are a variety of different machines that are used for radiation therapy and also different ways to classify the goal of the therapy. All of these factors impact the treatment protocol that your dog will receive.
“Traditional” or External Beam Radiation
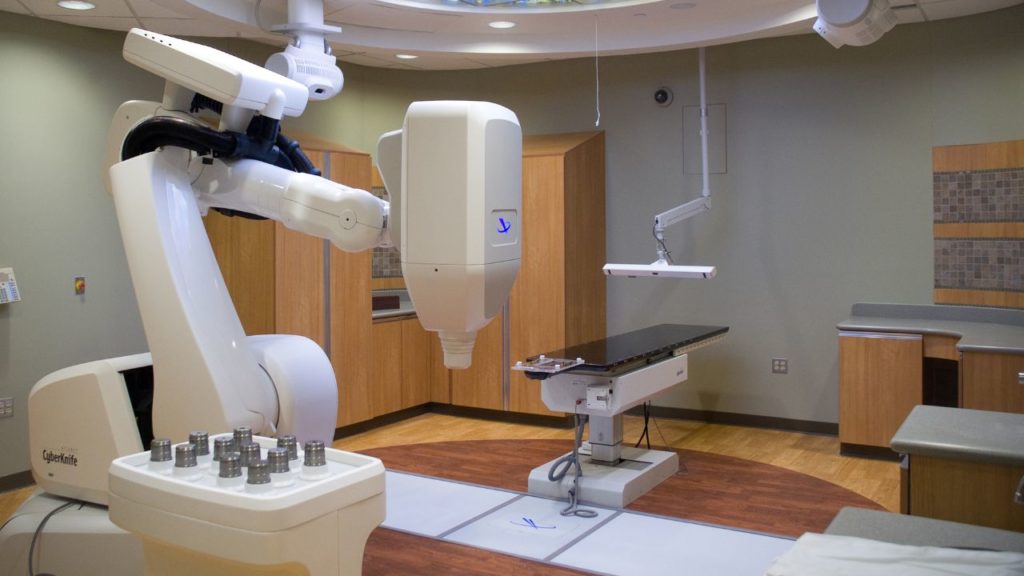
Radiation therapy in veterinary medicine usually uses something called external beam radiation. External beam radiation is created by a machine (often a linear accelerator) holding a radioactive compound. This advanced machine produces radiation from that compound and delivers it to the area with cancer.
Advances in radiation oncology have made the delivery of that radiation very precise, which limits negative consequences to surrounding healthy tissues.
3D Conformal Radiation and Intensity-Modulated Radiation
3-D conformal radiation therapy (CRT) and a newer technology called intensity-modulated radiation therapy (IMRT) are ways of forming or sculpting a field or target to appropriately receive the correct amount of radiation so the healthy tissue is spared from exposure as much as possible.
These technologies use CT images to make a map that shows how much radiation to give, and where. They still use a linear accelerator to produce the radiation beams but are more precise.
Stereotactic Radiation and CyberKnife
Stereotactic radiation therapy (SRT) is another more specialized type that allows the team to be incredibly precise with their calculations and target only the tumor, leaving healthy tissue alone.
The Cyberknife System is a very precise form of SRT technology that uses 1-5 treatments.2
Curative Intent and Palliative Intent
There are several different ways to deliver radiation therapy depending on the ultimate goal of treatment.
Curative or definitive intent means that the goal is to eliminate cancer or get as close to elimination as possible. This is used for dogs expected to do well for a long time after treatment.
Other situations warrant the use of palliative care radiation therapy. Palliative intent aims to decrease pain or improve function for an animal with severe or extensive disease where there is no curative option. While these patients may not gain long survival times, radiation therapy is still valuable because it can dramatically improve their quality of life.
Radiation Doses and Protocols
You may hear your veterinarian talk about a “dose” of radiation, but it doesn’t have quite the same meaning as a dose of a drug.
In radiation therapy, the amount of radiation administered throughout all treatments is called a “dose.” The unit used in radiation therapy is called the gray (Gy).
The amount of radiation given at each treatment is called a fraction. So, your dog will get a certain dose of radiation throughout therapy, given in fractions at each treatment.
Smaller Fractions = Fewer Side Effects for Curative Therapy
As precise as radiation therapy tries to be (see below), it’s very hard, and often impossible, to completely avoid irradiating healthy tissue. One of the reasons radiation therapy uses smaller fractions of the dose over time is to make sure healthy tissue isn’t too harmed by the therapy.
Most radiation therapy, especially in the context of curative intent, involves small daily doses (fractions) for each day of the week Monday-Friday, over a 3-4 week period.
These smaller dose fractions are better tolerated by surrounding healthy tissue.1
Larger Doses May Be More Desirable
Although small doses daily for multiple weeks are the most common curative method, there are treatment protocols that use larger doses of radiation that are administered further apart in time.
For example, stereotactic radiation therapy (SRT) generally breaks the overall dose into 1-5 fractions.1 The shorter course of treatment is attractive to many dog lovers if this technology is available.
Palliative intent radiation also often uses fewer, higher-dose fractions. Treatments may be done daily for a few days or once a week for a few weeks. This approach is less intensive for you to get your dog to appointments while still providing symptomatic relief for your dog. However, the higher fractions are more likely to cause long-term side effects.
Want to know what your dog goes through when he's getting radiation? Go 'in the back' with radiation expert Jenny Fisher in this special episode of DOG CANCER ANSWERS.
Planning Radiation for Dogs
Radiation oncologists want to be sure they are precise, so a fair amount of planning is involved in radiation therapy for dogs.
If your dog is getting radiation, planning might include:
- Bloodwork, and possibly chest x-rays, will be used to determine whether anesthesia is safe for your dog.
- Because radiation therapy requires extremely precise measurements of the treatment area, a CT scan is performed for planning purposes.
- Sometimes MRI is also used in the planning process.
This ensures that the treatment targets as much of the cancer tissue and as little of your dog’s healthy tissue as possible.
Usually, the first treatment is performed within days of this planning process to ensure that the measurements are as accurate as possible when the treatment is administered.
Your Dog May Get a Molded Positioning Device
Sometimes a precisely measured positioning device made of molding material is designed for your dog during the first treatment. This ensures that while treatment occurs, the body is positioned in the ideal fashion each time.
Perfecting the positioning can take a while, so your dog may be under anesthesia for an hour or more for this first treatment while the staff determines the best, safest position. The actual treatment time generally takes 5-7 minutes.
Once the ideal positioning for your dog has been determined and the mold is made, future radiation treatments will be much faster. That mold will be used each time your dog comes in, making positioning your dog quick and easy.
During Radiation for Dogs
Your dog must be under general anesthesia or heavy sedation for every radiation treatment. This ensures your dog is perfectly still and the radiation can reach its precise target. Once your dog is asleep, the team will position her according to their notes (or use the mold), administer the treatment (usually 5 to 7 minutes), and then wake her back up.
Is Radiation Painful for Dogs?
Radiation therapy is not painful at all.
However, your dog might be a little sore if she has to be in a weird position for the radiation to target her tumor.
He may also be groggy from the light anesthesia used during sessions.
Radiation Success Rate and Survival Data
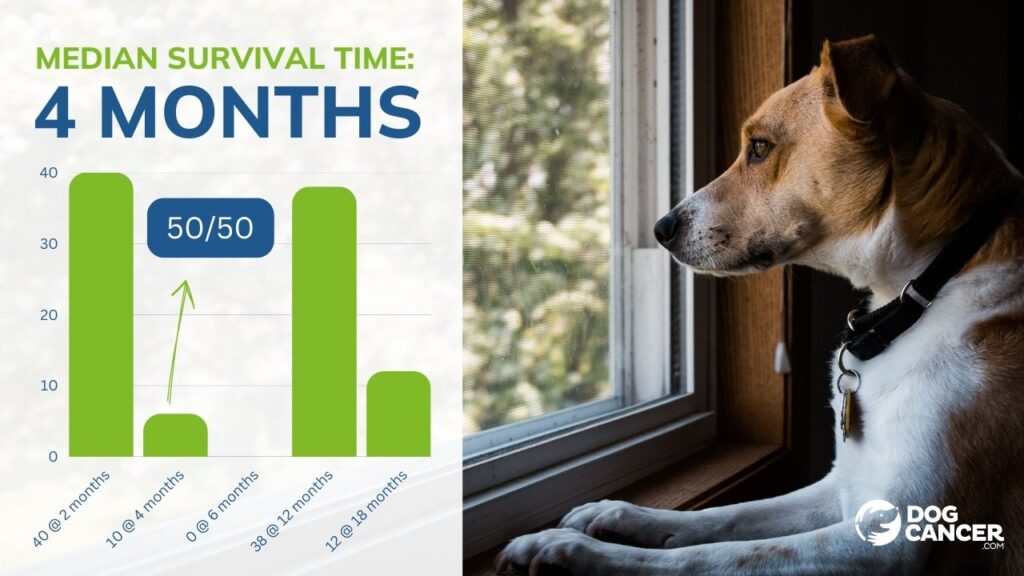
Radiation therapy generally improves cancer survival times due to its ability to kill cancer cells. Your dog’s exact survival time after radiation treatment will depend on the cancer type, therapeutic goal of therapy, and amount of disease.
However, generally, you can expect dogs who receive radiation treatment for cancer to live anywhere from 9 months to over two years.10,11
Some dogs that receive treatment for pain relief alone may live for less time, but for some tumors, radiation therapy can lead to 5 or more years of survival.
Soft Tissue Sarcoma and Radiation
For canine soft tissue sarcoma patients that receive surgery to remove a tumor and all but microscopic disease is removed, radiation therapy is extremely effective at killing those remaining tumor cells.
In these cases, “approximately 80-90% of dogs will respond to treatment and live for 3-5+ years without evidence of tumor regrowth.”7
Osteosarcoma and Radiation
For patients with bone cancer who are not good candidates for surgery in addition to radiation, survival time with radiation therapy and chemotherapy combined is about nine months on average.8
Radiation alone can also provide excellent pain relief for bone cancer patients.
The average survival time for osteosarcoma patients without treatment is about two months.11
Mast Cell Tumors and Radiation
Mast cell tumors may also benefit from radiation therapy. According to the Veterinary Specialty Center’s website, “radiation is most effective when the tumor cells remaining are in a microscopic setting (such as after surgery). With this protocol, approximately 90% of dogs will respond to treatment and live for 2+ years without evidence of tumor regrowth.”9
Overall, survival depends on several factors, but radiation therapy usually increases survival time and decreases cancer cells. This holds true for most “bulky” cancers with a distinct mass.
Nasal Tumors and Radiation
Nasal tumors are often only treated with radiation because surgery is extremely difficult in this area. Many dogs live about 1.5 years after treatment before their cancer returns.13
Radiation for Dogs Is Commonly Used for These Cancers
In addition to those listed above, radiation therapy is most used for treating:3
- brain and spinal cord tumors
- pituitary tumors
- soft tissue sarcomas
- mast cell tumors
- vaccine-associated sarcomas
- lymphoma
- nasal tumors
- oral tumors
- bladder tumors
- prostate tumors
- perianal tumors
- bone tumors
It can also be used for some tumors of the heart, lungs, and liver, though these areas are more difficult to target.1
How to Get the Best Results from Radiation for Dogs
Due to the level of specialty care that radiation therapy requires, following the recommendations of the oncologist (or total medical team) will provide the best results.
Preparation, supplements, and medication protocols are uniquely tailored to each patient, so ask your dog’s doctor specific questions about this.
Your dog will likely need to skip breakfast before radiation treatments. Ask the oncologist if you should give your dog’s regular meds on those days or skip them. Some radiation oncologists may ask you to bring food for them to give your dog after she wakes up.
Home Care After Radiation for Dogs
Home care specifics depend on the tumor type and patient status.
Cells of any healthy tissue close to or in the path of radiation can be negatively impacted. Your dog may experience skin irritation or irritation of the tissues in the nose, mouth, or eyes if these areas are within the radiation beam.
Wound treatments, gentle cleansing, bland food with low salt, or specific treatments for supportive care and pain relief may be needed to deal with these side effects.
If certain parts of the GI tract are affected, diarrhea or nausea and vomiting can also take place.
Your veterinarian will give specific instructions if your dog is at risk for these side effects. Similarly, if your dog is high-stress, you should also discuss possible ways of limiting anxiety during treatments.
Follow Up
Rechecks are typically based on any side effects your dog gets and rechecking target sites to measure how effective the treatment was. This is especially true when radiation is being used to treat a visible tumor or where radiation is the sole treatment method.
Depending on the cancer type, blood work monitoring may also be recommended to evaluate organ health and the risk of infection. Some repeat blood work may also be performed due to the number of anesthesia events that occur with curative intent treatment.
Follow-up appointments may be done at the radiation facility or your regular vet’s office, depending on the timing and how close you live to the radiation facility.
When to Not Use Radiation for Dogs
Radiation therapy is most effective for tumors with rapidly dividing cells; not all tumors respond to this treatment method. Some tumor cells can be resistant (or become resistant) to the impacts of radiation.
Radiation is also less likely to be effective for systemic cancers because only the cancer cells within the radiation beam will be killed.
Ask your veterinarian if radiation therapy is appropriate for your dog’s cancer type and extent of disease.
Where to Get Radiation for Dogs
Radiation therapy is only available through specialty practices. Veterinary radiation oncologists have extra training, education, and certification in this specific area.
The radiation equipment has very specific safety regulations. For example, an onsite physicist is required to maintain the machines. The equipment is incredibly expensive and is newer to veterinary medicine than it is to human medicine. For these reasons and more, the technology is mostly limited to larger specialty practices and university hospitals.
Machines capable of stereotactic radiation therapy are even less common.
Radiation for Dogs Safety and Side Effects
There are many safety guidelines for using radiation therapy due to the dangers of exposing healthy tissue to ionizing radiation.
You are probably familiar with some of the risks of radiation exposure from nuclear power plants, x-rays, etc. The advanced planning technology we use today for radiation treatments is much safer and more controlled than a reactor meltdown, but some things can go wrong.
Exposure to the same radiation we use to treat cancer can also cause cancer. It can also damage healthy tissue. This is why regulations and safety protocols around the use of radiation are so strict, and why facilities capable of housing this technology are few and far between.
The side effects of radiation therapy are divided into two categories. These categories are broadly referred to as early and late side effects.
Early Radiation Side Effects
These effects typically show up within the first two weeks of starting therapy and can continue for about one month after the total dose is delivered.
The early side effects most commonly impact skin or mucus membranes in the radiation field. Mucus membranes include gums, inner lips, or moist surfaces within the mouth or nose.
The visible changes you may see at home are typically redness, ulcers, increased salivation, or other indicators of irritation. The skin may change color or pigment, and fur or hair may fall out and have delayed or no regrowth.
Because sometimes the GI tract can be in the field of treatment, damaging the healthy cells in the GI tract can lead to diarrhea.
If the eye is in the treatment zone or is exposed, irritation of the eye’s surface and/or surrounding tissue is possible.5
There are supportive measures to help minimize the impacts of these side effects and decrease your dog’s secondary infection risk, so be sure to discuss these concerns with the doctor.
Late Radiation Side Effects
These effects happen more than six months (usually many years) after therapy and tend to affect the tissue that grows more slowly, in cells with slower turnover rates. This includes bone, nervous system tissue, and cartilage.
These effects are highly dependent on tumor type and surrounding tissue. Late side effects can also be seen as skin and muscle fibrosis.
Late side effects are less common than acute effects, and smaller single fractions with each treatment (dividing the total dose into smaller dose treatments) reduce these risks.
The likelihood of experiencing late side effects is less than 5%.6 Radiation-induced cancers are possible but extremely rare. If your dog is at risk for any specific long-term effects, your doctor will discuss these with you.
The Cost of Radiation for Dogs
The cost of a course of radiation therapy ranges from about $2,500-$10,000 depending on the number of treatments, the technology used, imaging requirements, dose, and severity of side effects.
CareCredit states, “Radiation, if necessary, can cost $1,000 to $1,800 for a palliative protocol, and $4,500 to $6,000 for curative intent protocol.”14
This number can be higher depending on where the treatment occurs and what advanced imaging and available technologies exist.
Topics
Did You Find This Helpful? Share It with Your Pack!
Use the buttons to share what you learned on social media, download a PDF, print this out, or email it to your veterinarian.