EPISODE 199 | RELEASED January 16, 2023
All About Anesthesia for Dogs | Tasha McNerney CVT
Anesthesia for dogs doesn’t have to be scary. One weird nap for your dog, one amazing opportunity for vets to provide lifesaving medical care.
SHOW NOTES
Tasha McNerney is a Veterinary Technician Specialist in anesthesia, and she’s sharing all the details on what your dog’s veterinary care team does to keep your dog safe, the things that can go wrong while under anesthesia, and what you can do to prepare your dog beforehand.
One of her best tips for dog lovers feeling anxious about an anesthetic event? Talk to your dog’s veterinary team. Ask about what training and credentials your state requires for someone to do anesthesia, as well as how the staff monitor dogs while under anesthesia and during recovery. Vets and vet techs all understand that you love and are worried about your dog, and hearing the protocols in place can help to ease your mind.
Listen in to learn about the different types of anesthesia and some of the different drugs that your vet will use to keep your dog calm and pain-free.
Links Mentioned in Today’s Show:
How ASA scores help make anesthesia safer for your pet patients https://www.veterinarypracticenews.com/how-asa-scores-help-make-anesthesia-safer-for-your-pet-patients/
[00:00:00] >> Tasha Mcnerney: If you take a patient that’s sick and fragile and then you layer in these anesthetic drugs, you can cause some big trouble. So we always wanna stabilize our patients as best as we can before going into anesthesia when it’s an urgent situation like that.
[00:00:14] >> Announcer: Welcome to Dog Cancer Answers, where we help you help your dog with cancer.
[00:00:20] >> Molly Jacobson: Hello, friend. Today on Dog Cancer Answers, we’re taking a deep dive into all things anesthesia, from the different types of anesthesia to why your dog needs it and why so many different drugs are listed on your invoice when your dog comes out of surgery or radiation. To explain all of this, our guest today is certified veterinary technician, Tasha McNerney.
Tasha McNerney, thank you so much for joining us today.
[00:00:48] >> Tasha Mcnerney: Thank you for having me.
[00:00:50] >> Molly Jacobson: You have a lot of letters after your name and I didn’t say them all, so why don’t you give me your letters and explain what they are.
[00:00:56] >> Tasha Mcnerney: Sure, sure. So first off, I’m a CVT, which is a certified veterinary technician. After I went to school for that degree, I became very, very interested in pain management, not only how we manage acute pain, but also chronic pain as well. So I became a CVPP, which is a certified veterinary pain practitioner. And then after that I was again, very interested in acute pain and like really getting down to the minutia of how we treat pain, especially surgical pain and pain under anesthesia, and how we maintain good anesthesia practices.
So I went and got my specialty. So I’m also a VTS or veterinary technician specialist in anesthesia.
[00:01:35] >> Molly Jacobson: Wonderful. So the equivalent in human medicine would be, say a nurse with a specialty in a specific area like anesthesia or pain management?
[00:01:45] >> Tasha Mcnerney: Yes, that’s correct.
[00:01:46] >> Molly Jacobson: Okay. Excellent. Well, I am so glad you’re here because one of the biggest fears that people have, whose dogs have cancer, is putting their dog under anesthesia. And as a trained specialist in anesthesia who happens to do most of the work associated with that, I would really love to hear your perspective on anesthesia for dogs in general, I wanna hear about what types there are, I wanna hear about whether or not dogs hear or feel anything while they’re under anesthesia, all of the questions that our listeners have, I know you can address. So where do you think we should best start? What’s the first thing you want people to know about anesthesia?
[00:02:32] >> Tasha Mcnerney: Oh man. There’s so many things. We probly could have like hours, hours, long conversation on this. But really to start, I want people to know that there is a risk with anesthesia, right? Anesthesia is risky. But that doesn’t mean that there aren’t a lot of things that we can do in veterinary medicine to minimize that risk.
Now a lot of it’s gonna go, uh, play into what is the ASA, or American Society of Anesthesiologists, kind of risk factor that we assign to that animal. So that’s gonna be a huge thing to just assign a risk factor to that animal.
[00:03:03] >> Molly Jacobson: And that’s something that you can do. You can actually take a look at the dog’s history and age and all – what goes into that risk factor?
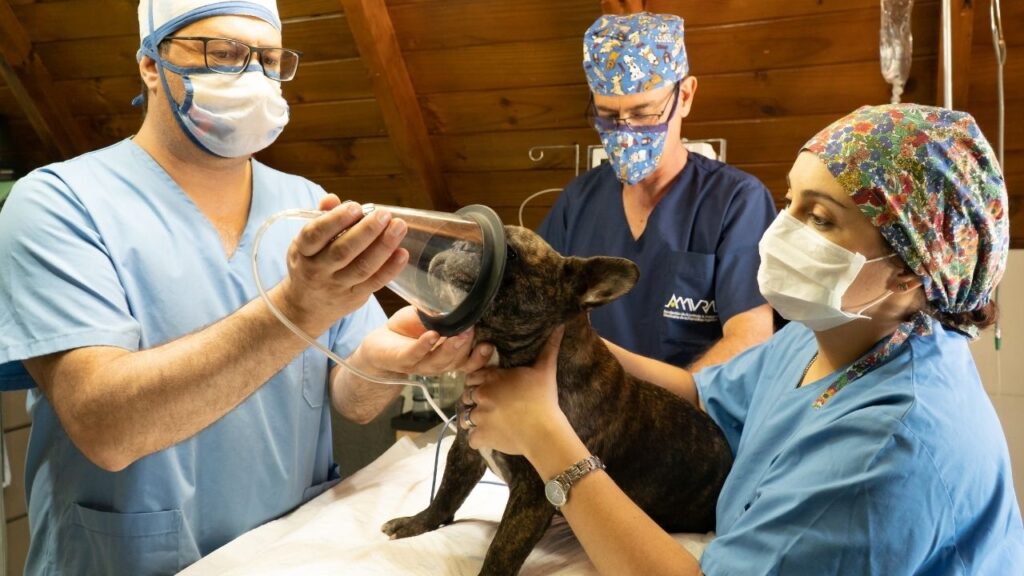
[00:03:11] >> Tasha Mcnerney: So we look at things like age, we look at things like concurrent disease status. Are they cardiovascularly healthy? Are they pulmonarily healthy? Are they able to ventilate well, you know, on their own? And that’s why, you know, breeds like English Bulldogs or French Bulldogs are just gonna have a higher risk factor than other breeds, you know, like than the Labrador, because those animals based on their body conformation already have a harder time ventilating.
So when we put them under anesthesia, that increases their risk. Now, I’m not saying that we should never put French Bulldogs or English Bulldogs under anesthesia, it just means that if you’re going to put them under anesthesia, you need to know the associated risks with a breed like that under anesthesia.
So breed does go into our ASA risk factors. Things like recent blood work, are there any liver abnormalities? Are there any kidney abnormalities? All those things like that. And this doesn’t necessarily go into the risk factor, but something that we wanna keep in mind as veterinary professionals is how long is this procedure going to be?
Certainly the number of hours under anesthesia means that we are at greater risk for complications that come along with anesthesia. What is the training level of the people who are gonna be monitoring that anesthesia? This is a big, big thing for me.
[00:04:26] >> Molly Jacobson: As someone who’s trained.
[00:04:27] >> Tasha Mcnerney: Because I am so, so stupidly trained, um, but at the same time, you know, I think that most people don’t realize that in most states you do not have to be certified or licensed to monitor an animal under anesthesia. You really could be working at Starbucks one day, and this is not anything against people who work at Starbucks, this is just saying you really could work in any industry one day and the next day be putting animals under anesthesia. That contributes to risk. Right?
So I think one of the things that I like to tell people is get to know who is going to be the one monitoring your patient under anesthesia, or your pet under anesthesia. And that’s because during surgery, the veterinarian is occupied. The veterinarian is performing a surgery. Their mind is taking out that tumor in the abdomen, amputating that leg, right? So their mind is focused on that. So who is the person who is gonna be focused on your pet under anesthesia? That adds to risk as well.
Is it somebody who is trained and has years of experience? Is it somebody who is brand new and maybe doesn’t have that level of training? That’s an important question to ask your veterinarian before anesthesia.
[00:05:40] >> Molly Jacobson: Wow. It never occurred to me. And I’ve actually had people tell me that in small practices sometimes the vet is the person who’s doing the surgery and also monitoring the anesthesia.
[00:05:50] >> Tasha Mcnerney: Yes. That’s not optimal, unfortunately. And that’s just because as humans, right, we think we can multitask, but we really can’t. And here’s the thing, if your doctor, your veterinarian, again, their main focus is to be in the surgery. So if they have their hands in the abdomen and they’re doing something and they see a massive arrhythmia pop up on the screen, now what do they do with their hands in the abdomen?
They have to call somebody else to come in. So optimally it’s best if your surgeon is focused on what they need to do surgically, and you have a trained anesthesia technician solely focused on the anesthesia of that patient.
[00:06:27] >> Molly Jacobson: Okay. There’s a lot of places I wanna go. I wanna know what could go wrong, like what the actual risks are, what could happen, and then I wanna know what kinds of things you do to take care of the dog if those things go wrong. And I wanna know how things typically go. Like are we focusing on the worst case to make sure that everybody understands the risks, but how common that is.
[00:06:51] >> Tasha Mcnerney: It’s not as common. So full disclosure, in veterinary medicine, we do have a much higher mortality and morbidity rate than human medicine. Now, a lot of factors go into that. Some of those factors are that we make a lot of preoperative testing for dogs optional. So maybe before you go under anesthesia, your doctor would say, Hey, Let’s do some radiographs, let’s do an echo, make sure your heart is healthy for this.
Dogs, we don’t usually do that. We can ask the people if they wanna do an echocardiogram and check the health of the heart before anesthesia, but it doesn’t always happen. And again, that’s, that’s fine. A lot of animals maybe don’t require it. But if you have a senior patient, um, like perfect example is a senior Boxer that is, you know, maybe needs to have an abdominal tumor removed. They should have an echocardiogram beforehand just because again, that breed is more predisposed to cardiac abnormalities, such as dilated cardiomyopathy.
So before we put them under anesthesia and increase that risk, we wanna know kind of what are we dealing with. So any information that we can get before the anesthetic event happens is just gonna be to the benefit of the patient.
[00:08:01] >> Molly Jacobson: Okay.
[00:08:02] >> Tasha Mcnerney: Now, echocardiograms are expensive, so not every canine owner can afford to get an echocardiogram. So the next best thing is to have your clinician do a full, as best they can, cardiac exam on the patient. We’ll run an ECG. We will have our clinician listen to them to evaluate for any possible murmurs. We’ll feel peripheral pulses to make sure they match and that kind of thing. So those are things that we want to do before our patients undergo anesthesia.
And to kind of kind of circle back to what you were saying before, it’s not that common. So I don’t wanna scare people. Even though our risk is higher in veterinary patients than in human patients, it’s still not that common. I’m gonna knock on some wood here or whatever I can ’cause I’ve been doing this for 16 years. And while I can’t say that I have had no anesthetic deaths, in the course of 16 years in doing anesthesia and in anesthesia for that full time, I’ve had about four anesthetic deaths over the course of my career. So I can’t say that it doesn’t happen, but it’s not common.
[00:09:04] >> Molly Jacobson: Okay. And how many dogs total would you say that you’ve worked with?
[00:09:08] >> Tasha Mcnerney: Oh my gosh. Oh my gosh, it’s so hard to say, hundreds. Hundreds, hundreds.
[00:09:13] >> Molly Jacobson: Okay.
[00:09:14] >> Tasha Mcnerney: Only because there are days that, you know, early in my career when I was working at a very high volume practice, I could be doing six dogs a day. At one point we worked with a Greyhound rescue that would bring them up from Florida, and we would do a lot of work with them. So we would have so many dogs in one day. Nowadays that I work more in, uh, a specialty practice where everything is very specialized and very hyper-focused, I probably only have one to two patients per day instead of the six per day.
[00:09:42] >> Molly Jacobson: Okay.
[00:09:42] >> Tasha Mcnerney: Which actually I like. I’m okay with that pace. It lets me like really focus in on the patient.
[00:09:47] >> Molly Jacobson: Yeah, that makes sense. So when things go wrong, what are they? What are the things that are going wrong?
[00:09:53] >> Tasha Mcnerney: Yeah, it’s a great question. So usually the things that are gonna go wrong under anesthesia have to do with the hypos, as we call them. Hypotension, hypoventilation, and hypothermia.
[00:10:05] >> Molly Jacobson: And hypo means?
[00:10:06] >> Tasha Mcnerney: Hypo means low, right? So again, we have hypothermia or low temperature, hypoventilation where we are just not getting rid of the CO2 that’s building up in the body and exchanging it for oxygen. And hypotension, which is where we have low blood pressure, right? And we really care about that one. We’re pretty hyper focused on our blood pressure during anesthesia because we look at our blood pressure, our blood pressure in itself is what’s going to be responsible for taking the blood where it needs to go, going to all the parts of the body, going to all the major organs. We need a blood pressure to be a certain number to get blood where it needs to go so we can deliver that oxygen. If our blood pressure is really low, that means that major organs are gonna be without oxygen. And that’s why when dogs come in and they are very, very sick, sometimes you might see this with your hemangiosarcoma patients that end up having a hemo abdomen, right?
Where that splenic tumor is now bleeding into the abdomen and all of the blood that’s carrying the oxygen is not able to go to the tissues because it’s sequestered in the abdomen.
[00:11:13] >> Molly Jacobson: Right.
[00:11:13] >> Tasha Mcnerney: So those animals usually come to us already very sick. They’re low on oxygen. Those major organs are not getting the oxygen it needs. So again, those are a high risk to put under anesthesia. We really wanna, if I have an animal like that come into the clinic, you know, we’re usually gonna take those animals to surgery to remove that splenic tumor, but because they come in really sick, we need to stabilize them before anesthesia.
Like one of the things we don’t wanna do is just rush into anesthesia without stabilizing, ’cause if you take a patient that’s sick and fragile and then you layer in these anesthetic drugs, you can cause some big trouble. So we always wanna stabilize our patients as best as we can before going into anesthesia when it’s an urgent situation like that.
[00:11:55] >> Molly Jacobson: And stabilizing might be what?
[00:11:57] >> Tasha Mcnerney: So stabilizing is usually, again, because those patients come in where they are hypotensive, right? They don’t have enough circulating blood volume because all of that blood is sequestered in the abdomen. So for those patients, we need to fix that hypotension as best as we can before we get into the OR. We might wanna provide some supplemental oxygen to those patients. We might wanna blood type those patients as well to make sure that we have blood products ready for them, again, to give them a little more of circulating blood oxygen carrying capacity for them.
We also wanna provide pain management to them. If any of you guys listening have ever had just like deep abdominal pain, you know that it hurts. So we wanna make sure that we’re providing pain control to these patients as well, because the pain control is gonna be a really important component to making sure that they’re calm and they’re stable before we get into surgery.
[00:12:50] >> Molly Jacobson: Okay. So it sounds like there’s a lot that goes into anesthesia that maybe-
[00:12:55] >> Tasha Mcnerney: Yeah.
[00:12:55] >> Molly Jacobson: -the average person doesn’t really understand ahead of time. So what should we be doing at home, if anything, to prepare our dogs?
[00:13:05] >> Tasha Mcnerney: So, interestingly enough, we have some really cool things that you can do at home that are kind of coming to the forefront, or at least in the past couple of years, are becoming more popular, I would say. And one of these things is the thought of pre-visit pharmaceuticals. Now, of course, if you are coming in as an emergency surgery or anesthesia patient, this is a little bit different, we’re not able to do this. But let’s say you are that, you know, 10 year old Greyhound that may have a osteosarcoma and we’re going to do a limb amputation and we have it scheduled.
Some of the things that we can do for these patients is provide preemptive kind of calming medications. We know that for dogs to come into the hospital, you know, any dog, even if it’s a calm, stoic, Greyhound, as they usually are, it’s still stressful for them. There’s a lot of sounds. There’s a lot of interesting smells. They’re away from their owner, they’re away from home. So this can be really stressful for them.
And when it’s really stressful for them and their heart rate gets going and they get really nervous, that actually kind of sets us up for needing more anesthesia.
[00:14:13] >> Molly Jacobson: Ha.
[00:14:14] >> Tasha Mcnerney: And that’s what I don’t want, right? My whole job in anesthesia is to provide kind of a layered balanced of different drug classes so I don’t have to use just one whopping dose of a drug. ‘Cause anytime I have to use a big whopping dose of a drug, I’m gonna have bigger side effects. So that’s what I wanna minimize. So there’s this kind of notion in, uh, veterinary medicine in the past few years, this kind of notion of low stress handling. And that’s where we’re going to try to treat the animals as calmly as possible.
And we don’t wanna wrestle dogs down anymore to try to place IV catheters. We wanna give them a little bit of something that’s gonna take the edge off at home, right, so it gets into their system. So usually a couple hours before planned surgery, we will have an owner administer a dose of these sedatives.
Now your doctor might prescribe a sedative such as Trazodone. They might prescribe something like Gabapentin. Either one of these drugs helps as a sedative to just calm the patient so that way when they come in to us and it’s time to place their IV catheter, they don’t have that level of fear and anxiety that happens that’s just gonna make me need to use more anesthetic drug.
So if we can give ’em a little bit of sedation to kind of take the edge off, that’s what we wanna do. And I think that’s one of the things in the past five years in veterinary medicine that’s been monumental. Especially when it comes, again, just the fear and anxiety in the animals, they recover from anesthesia much better, much calmer, and they make my job easier if they come in already having a little bit of sedation at home, because again, then I don’t have to use a whopping dose to get them sedated for anesthesia, to have them place a catheter.
So that’s one thing. At home, you can administer these doses of drugs, and this usually is something that your veterinarian will prescribe based on, again, breed, age, body size, et cetera.
[00:16:04] >> Molly Jacobson: Okay.
[00:16:05] >> Tasha Mcnerney: But they usually will give you a dose to give a couple hours before you come in for surgery, and that makes a big difference.
[00:16:11] >> Molly Jacobson: Is that common practice now to prescribe these ahead of time?
[00:16:14] >> Tasha Mcnerney: It’s pretty common practice where I am located on the East Coast. So most large specialty practices, most surgical practices around, you know, New York City, Philadelphia, Washington DC, and at most of the universities and veterinary teaching schools are pretty on board with this.
Again, things move slowly in veterinary medicine just as they do in regular medicine. So it’s taking a little bit for it to kind of reach probably like rural Michigan or you know, maybe somewhere in the mountains of Colorado. Um, but it is becoming more commonplace. Again, which is only gonna benefit the patient itself.
[00:16:51] >> Molly Jacobson: Absolutely. It sounds like something that if our listeners are looking at or planning a surgery, they should ask about if it’s not already talked about.
[00:16:59] >> Tasha Mcnerney: Oh, 100% yes. Again, there are a couple of different drugs that we can choose, so sometimes they might even do a combination of a drug like Gabapentin and Trazodone, but Trazodone is pretty much the most common one that we use as a preemptive anxiolytic for our canine patients.
[00:17:16] >> Molly Jacobson: Mm-hmm. Great. So once the dog is calm and brought in for a planned surgery, not an emergency surgery, what’s it like for you as the anesthesiologist in the room, for lack of a better way of putting it?
[00:17:31] >> Tasha Mcnerney: Yeah, almost. So I will clarify that I’m a technician specialist in anesthesia, and-
[00:17:36] >> Molly Jacobson: Right.
[00:17:36] >> Tasha Mcnerney: -that means I function kind of similarly to a human RN or a nurse anesthetist. And then at some practices, especially university teaching hospitals, et cetera, they do have veterinary anesthesiologists. So, they have kind of really high level people who have spent the past eight years, you know, doing nothing but anesthesia and veterinary anesthesia specifically.
So if you have the opportunity to take your canine to a place that has a boarded anesthesiologist, that’s always gonna be the safest bet. But again, if you’re like my dad who lives in rural Michigan and doesn’t have access to that, then having someone on staff, just talking to your veterinarian and asking them do they have somebody on staff who potentially is a technician specialist in anesthesia, or even just a technician who’s trained in anesthesia and anesthesia monitoring.
But what it’s like for me is, I mean, it’s awesome. Uh, I guess like I wouldn’t be doing it for 16 years if I didn’t find it awesome and fascinating and personally rewarding. I think that every veterinary professional gets into this job because we want to ease animal suffering. And for me, if I know that I can help devise a drug plan that is going to keep this patient as comfortable as possible, as pain free as possible, to allow the surgeon to get done what they need to get done in the most timely manner possible, and then ease recovery of that patient.
But then also the client interaction, right? I wanna talk to the clients. I know that this is a difficult decision for them, right? Having a patient undergo anesthesia is scary, is worrisome. They’re fearful. So I wanna talk to them. Here are some ways that we can minimize that, here’s how we can work together to make sure this recovery is as smooth as possible. All of those things.
So I really find it very rewarding, and I think for me, especially, you know, especially animals that come in that maybe are one day not walking, especially not eating at all, and then they come in and they have a procedure done and then you talk to the owner and a couple weeks later they’re back to eating again. And one of the best comments that we get is, oh, he’s like a puppy again. Like, that’s really fantastic. And that’s what I wanna keep perpetuating.
[00:19:56] >> Molly Jacobson: Because what your role is really is to make it possible for that quality of life or lifesaving procedure to happen, with a minimum of stress for the dog. Because the point of anesthesia really is to make it so that you don’t, are not aware of what’s going on on the surgery, but someone’s cutting you open.
[00:20:14] >> Tasha Mcnerney: Correct.
[00:20:15] >> Molly Jacobson: So that, yeah. So how do you make sure that that happens? Like, I wanna hear more about, like do you literally make a different plan for every animal that you help?
[00:20:26] >> Tasha Mcnerney: Yes. Uh, I think that’s why I’m really drawn to anesthesia is that I like puzzles, right? And if you present me with a patient, here’s your patient, and then also, here’s the procedure they’re having done. So here is a set of facts about this patient. Here is a set of rules and facts about the procedure they’re having done.
Now look at the anesthetic drugs you have available to you, and you’re going to pick what is gonna make the most sense to plug in for this particular patient having this particular anesthetic event and this particular pain level. So if there is an animal that comes in that maybe, you know, they jumped over a fence, they have a small laceration, that is going to be treated much differently and have a much different drug protocol than, let’s say, again, that sight hound that comes in that has a tumor and we need to do a front limb amputation.
Right? So the level of analgesia involved is gonna be much different. I would say for the most part, a lot of the things – not a lot, some of the things are the same. We always wanna have an analgesic component to our drug protocol and a sedative component to our drug protocol. Almost everything for veterinary patients is done under general anesthesia, which means that we are placing a tube down their throat and delivering anesthetic gas to keep them fully asleep.
In human medicine, we can do a lot of things under local-regional anesthesia, which means that you could potentially have abdominal surgery, for instance, I had a C-section, I was under spinal anesthesia, so I was fully awake, but my abdomen was completely open, but I felt nothing.
[00:21:55] >> Molly Jacobson: Right.
[00:21:55] >> Tasha Mcnerney: We can’t do the same thing with dogs, unfortunately, you know, they will not just stay still while we open up their abdomen, ’cause they, they just don’t understand what’s happening.
[00:22:03] >> Molly Jacobson: Right.
[00:22:03] >> Tasha Mcnerney: So they have to be fully under anesthesia, and that’s where we have to use the anesthetic gas. And that’s kind of where it changes a little bit because anytime we present anesthetic gas into the equation, anesthetic gas is one of those things that is responsible for major hypotension.
[00:22:21] >> Molly Jacobson: Ah, I see.
[00:22:21] >> Tasha Mcnerney: Right. So the thing that we’re worried about. So when I said that we’re picking and choosing all these different drugs to add in, right, what we could do is certainly we could give this animal a whopping dose of anesthetic gas, and they would stay asleep and their brain would be offline. However, that’s not in the best interest of the patient.
So what I wanna do is give them a little of IV opioid, right, to help them with some pain control. I might give them some IV adjunctive drug, you know, something that’s gonna provide a little sedation. You know, if anybody in the audience has ever had like, Versed or Midazolam or a Valium or something like that, we can give them a little bit of that IV to help calm them. And then we can layer in the anesthetic gas, right?
We don’t wanna just go full on with the anesthetic gas, ’cause that’s not in the best interest of the patient’s blood pressure, which means it’s not in the best interest of delivering oxygen to the liver, the kidneys, the heart, and the brain.
[00:23:14] >> Molly Jacobson: I see. So you’re using those calming and sort of pain killing things to make sure that anesthetic doesn’t have to do all of the work. It doesn’t have to keep the body still and relieve pain and relieve anxiety, which it will if you use enough.
[00:23:28] >> Tasha Mcnerney: Correct.
[00:23:29] >> Molly Jacobson: But you wanna use these.
[00:23:31] >> Tasha Mcnerney: Yes.
[00:23:32] >> Molly Jacobson: But you don’t wanna use that much. So you use other medications to take care of two of those things so that you can use a lower dose of the anesthetic just to keep the body’s – am I getting it right?
[00:23:43] >> Tasha Mcnerney: Yep. You’re getting it right. And then there’s also kind of this misconception that I just wanna make sure everybody’s aware of, and that’s that anesthetic gas is going to kind of turn the brain offline, right?
[00:23:54] >> Molly Jacobson: Right.
[00:23:54] >> Tasha Mcnerney: But anesthetic gas in itself is not providing analgesia. Now, the only anesthetic gas that we have that will provide analgesia is nitrous oxide, but that’s not commonly used in veterinary medicine. But if we’re using one of the more common anesthetic gases in veterinary medicine, that will provide anesthesia, but it does not provide analgesia or pain control.
And that’s why a preemptive dose, when I give them a little bit of morphine IV or I give them a little bit of maybe even something like ketamine, we do use kind of like small doses of ketamine in veterinary anesthesia for its pain control properties.
So we wanna make sure that we’re layering in pain control together with the anesthesia. Because yes, we could just turn on that anesthetic gas to a very high level and the patient wouldn’t move, they wouldn’t react. But the problem is when that anesthetic gas goes off, guess what happens? All of those pain receptors are now flooded with signals.
[00:24:47] >> Molly Jacobson: Oh.
[00:24:48] >> Tasha Mcnerney: Which again, we don’t want.
[00:24:49] >> Molly Jacobson: I see.
[00:24:49] >> Tasha Mcnerney: We wanna make sure that we have some analgesic in the body, some opioid or some local anesthetic or something like that in the body so that when that gas goes off, those pain receptors aren’t bombarded.
[00:25:01] >> Molly Jacobson: That makes a lot of sense. So that’s one of the main things people worry about too. They worry, two things, their dog’s not gonna wake up, which you’re addressing by using as little anesthesia as you can to get the job done, right?
[00:25:12] >> Tasha Mcnerney: Yes.
[00:25:13] >> Molly Jacobson: And then the second thing is, is my dog aware of what’s going on and is my dog in pain? And those other medications will sort of take care of that. So this layered approach is doing all of that?
[00:25:24] >> Tasha Mcnerney: Yes. And that’s what you want. So I do encourage people that if your animal is about to undergo a surgical procedure, you talk to your veterinarian. Hey, what kind of pain control do you guys use preemptively before they’re under anesthesia? How long of an anesthetic procedure is this going to be? And one of the things, especially if the patient is having any kind of dentistry work done or advanced dental work, um, ’cause sometimes for some of these oral tumors, we might have to remove a section of the jaw.
[00:25:52] >> Molly Jacobson: Right.
[00:25:53] >> Tasha Mcnerney: So you wanna talk to the doctor and say, Hey, is there gonna be local anesthetic on board? Right? Because if you went to the dentist and you had a tooth removed, they would numb up your jaw, et cetera. So we wanna make sure we’re doing the same thing for our canine patients if they’re about to have a tooth extracted or a piece of their jaw extracted. We do a lot of local anesthetic for our patients.
[00:26:13] >> Molly Jacobson: So you do local anesthetic at the same time as you do the general anesthesia.
[00:26:17] >> Tasha Mcnerney: Correct.
[00:26:18] >> Molly Jacobson: I see.
[00:26:19] >> Tasha Mcnerney: Now, and there’s some people that would say, well, why do you need to do the local anesthetic if they’re not feeling anything because of the general anesthetic? And that’s because, again, once that general anesthetic goes off and their brain is back online, we don’t want all of the pain coming from their tooth or their jaw like going into their, their brain, right? We don’t want all of those signals going. And the local anesthetic is gonna block those signals from going up into the brain.
So local anesthesia is a, a huge component of kind of this theme of balanced anesthesia and appropriate pain control.
[00:26:51] >> Molly Jacobson: Okay, let’s take a quick break and when we come back I wanna ask you, Tasha, about reversible anesthesia.
And we’re back with Tasha McNerney. There’s something called reversible anesthesia. What does that mean?
[00:27:09] >> Tasha Mcnerney: Yeah, so it’s pretty fascinating. Um, and again, one of the reasons I really love anesthesia in itself is I really love pharmacology and physiology. And there’s this concept that a lot of these drugs that we ask them to go to receptors and make an action happen, right?
So you can give a patient an opioid drug and that will kind of reduce the perception of pain in their system. It will kind of subdue those pain fibers that are sending off these signals. But there’s another drug class that you can use that will go to the same receptors as the opioid and they’ll go up to the opioid and they’ll just go, boop, and they’ll kind of kick them off the receptor. So they reverse the effects of the opioid.
There’s another drug class called Alpha-2 agonists, and they provide sedation and analgesia. It’s a fascinating drug class, and if anybody really wants to get in depth, there’s a lot of really cool articles out there about drugs like Dexmedetomidine and Medetomidine we use a lot in veterinary medicine because they’re so reversible because we have the drug and then we have, basically the reversal, in one bottle.
So if we get into trouble under anesthesia and we notice that maybe things aren’t going right, we need to abort this mission, we have a way to effectively give an IV reversal of that drug, which is pretty cool.
[00:28:35] >> Molly Jacobson: That’s really interesting. So there are anesthetics that you can use specifically so you can turn them off really quickly.
[00:28:43] >> Tasha Mcnerney: Yes.
[00:28:44] >> Molly Jacobson: That’s really cool. You mentioned inhalant, like the tube down the throat, that literally is gas, right? That they’re inhaling?
[00:28:52] >> Tasha Mcnerney: Yes.
[00:28:52] >> Molly Jacobson: I know there’s local anesthetic, which is, you’re just injecting, you’re giving, basically using a needle to insert it. And then there’s injectable, and you just mentioned sometimes these reversibles are injectables. Is this the same or is there other?
[00:29:07] >> Tasha Mcnerney: Yeah, so a lot of people will talk about, or if your, your veterinarian mentions to you that we’re gonna use injectable anesthetics, usually that’s things like these reversibles that I talked about, Alpha-2 agonist, Dexmedetomidine, Medetomidine, et cetera. Or they might utilize an injectable anesthetic, something like Propofol, right, or um, Alfaxalone.
[00:29:26] >> Molly Jacobson: Okay.
[00:29:27] >> Tasha Mcnerney: So these drugs are basically, they’re different than analgesics. These drugs in themselves are able to get a patient where they – if anybody has ever had like twilight anesthesia-
[00:29:40] >> Molly Jacobson: Uh huh.
[00:29:41] >> Tasha Mcnerney: -right? Where they gave you an amount of anesthetic, and you’re not all the way out, right?
[00:29:45] >> Molly Jacobson: Right. You don’t really know what’s going on.
[00:29:47] >> Tasha Mcnerney: You don’t really know what’s going on, your brain is somewhere else, right? In a field, eating donuts, whatever you’re doing. But we use those injectable anesthetics sometimes to kind of bridge the gap between just giving a pain reliever and then getting the tube down the throat. Because the thing is, we can’t just take an animal, open up its mouth and it’ll let us put a tube down its throat.
It needs to be pretty out before we can do that. And usually we use these injectable anesthetics to bridge the gap between our opioid analgesic and our gas.
[00:30:20] >> Molly Jacobson: I see.
[00:30:20] >> Tasha Mcnerney: So we need something to help us get the tube down the throat. And usually that’s something like Propofol is probably one of the most common ones we use.
[00:30:27] >> Molly Jacobson: So when you get your bill after one of these surgeries and you see all of these medications listed, there might be several of those that are actually the anesthetic agents or the medications that were prescribed and used during the surgery just to manage all of this.
[00:30:42] >> Tasha Mcnerney: All correct. Yes.
[00:30:43] >> Molly Jacobson: Okay. So once you turn the gas off and they start to wake up, what’s that like for the dog?
[00:30:50] >> Tasha Mcnerney: Yeah, so there’s two, in anesthesia land, we say that there’s two really critical points of anesthesia. Usually it’s not maintenance, uh, usually it’s not during the surgery, again, unless the patient is really critical. But usually it’s during induction, right? That first moment where we’re giving drugs, putting the tube down the throat. And then the second area where we really have to be careful and very watchful is recovery, right?
Because recovery from anesthesia for some animals can be a very smooth, calm process. But for some animals, especially animals who may not have had a pre-visit sedation, or if you have a patient that you know is just very high strung, very fearful, or has any kind of fear aggression, for them, it can be really rough to wake up, you know, from a, from a sleep to a place where there’s again, there’s strange smells, there’s strange noises, there’s people you don’t know. It can be a really rough time for them. So again, we have drugs that can mitigate those rough recoveries. But for me, recovery is one of those areas that I’m really hypervigilant. And again, if I have certain breeds, our brachycephalic breeds, right? Our Boxers, our French Bulldogs, our English Bulldogs, anything that has that smushy face – I can’t believe I didn’t say Pugs, ’cause Pugs are my favorite. That is my favorite breed of dog.
But anything with the, the kind of smushy face, we have to be really hypervigilant because for them when they’re awake, just their physiology, they have learned to compensate for the fact that they can’t bring in a lot of oxygen. They’ve just learned to compensate.
But when we give them anesthetics and analgesic drugs, we take away their natural ability to compensate, which means that during the recovery period, we have to be very vigilant with brachycephalic breeds because we need to basically sit there with them until they’re kind of moving their head around and they’re kind of swallowing and they’re able to oxygenate themselves.
One of the worst things that we don’t wanna do is just be like, oh, yep, surgery’s over, put ’em in a recovery cage and then walk away. Brachycephalic breeds can quickly desaturate, which means that their oxygen levels can drop very quickly because again, without their compensatory mechanisms, they can’t bring in that oxygen.
[00:33:08] >> Molly Jacobson: Do you keep oxygen on them?
[00:33:10] >> Tasha Mcnerney: Yes. So oftentimes with brachycephalic braids, we have a little portable unit that will give us a pulse ox reading or pulse oximeter reading, so it’ll tell us the percentage of oxygen being carried on that patient’s hemoglobin. So I like to keep a portable pulse ox on those patients in recovery. I like to keep extra intubation materials, which means that if this patient went into crisis, I am able to put a tube down its throat very quickly and administer supplemental oxygen.
And then sometimes for some patients, we also will do nasal cannula oxygen. So for instance, if we have done a maybe thoracic procedure and we have taken out a lung lobe, and now we know that their oxygen carrying capacity and their ventilation capacity is reduced, in the recovery period, we’re watching those guys really closely. We’re providing supplemental oxygen. We might be providing additional sedative drugs to keep them calm.
Right? Because especially if a patient has had any kind of thoracic or respiratory procedure, as they get worked up and really anxious and they’re breathing faster, they can tend to hyperventilate themselves and basically pass out. So we don’t want that either.
[00:34:17] >> Molly Jacobson: Right, right, right. So there’s a lot, you know, like when they say, okay, the surgery’s over and she’s in recovery, there’s all of this stuff still happening.
[00:34:26] >> Tasha Mcnerney: Oh, yes. Yeah. Just because the gas is off, right, just because the inhalant gas is off and the patient is all sutured up and it looks nice, that doesn’t mean our job is over. We still have recovery to get through and recovery, again, for most patients, recovery is just another we’re gonna make sure that we get them warmed up after surgery, that they’re oxygenating properly after surgery. And then for some patients that are maybe staying overnight in the hospital, we wanna make sure that their pain level is taken care of.
So we are always going back in and checking their pain scores and evaluating that and providing additional analgesics as needed. We wanna make sure that those patients are up and eating normally. Now, I’ll say up and eating normally, but as you guys, you know, probably know, an animal that’s in an unfamiliar environment that maybe just had abdominal surgery is usually not too keen on eating a huge meal. Maybe unless they’re a Labrador, right? Because a Labrador-
[00:35:20] >> Molly Jacobson: Labradors are always in the mood to eat.
[00:35:21] >> Tasha Mcnerney: No matter what happens, that Labrador is gonna eat dinner.
[00:35:24] >> Molly Jacobson: So how long does it generally take a dog to wake up enough to go see mom?
[00:35:30] >> Tasha Mcnerney: So it depends on the procedure that has happened. If it’s an orthopedic procedure, those ones usually do have a longer recovery and that’s usually because the orthopedic procedures we’re using more advanced and longer lasting regional blocks. Like for instance, if you have a dog that needs to have a hind limb amputation, they are going to have an epidural. And epidurals can then last anywhere from six to eight hours.
So we wanna make sure that that epidural has worn off enough that the dog can urinate on its own, because we know that epidural analgesia can affect the bladder and they can have some urine retention. So we wanna make sure that they are able to ambulate, they’re able to urinate on their own, and then they can usually go home.
Now a lot of practices will like to keep orthopedic procedures overnight, again, to make sure that their pain is being controlled appropriately, to make sure they are able to ambulate, especially if they’ve had an amputation and now they’re going around on three legs, um, which amazingly enough, dogs just do so fantastic. It’s usually, I’m always amazed at how well dogs can compensate with three legs, really.
[00:36:37] >> Molly Jacobson: Yeah.
[00:36:37] >> Tasha Mcnerney: Um, but we like to keep an eye on them. If it’s a more stable procedure, I would say, those ones will usually go home anywhere between, you know, three to five hours of coming off the table.
[00:36:50] >> Molly Jacobson: Okay. And every time I’ve ever taken a dog back from surgery, they’re still pretty dopey when I get them back.
[00:36:56] >> Tasha Mcnerney: Oh yeah.
[00:36:56] >> Molly Jacobson: How long will that kind of dopiness last?
[00:37:00] >> Tasha Mcnerney: So it’s different for every patient. I know, that’s the anesthesia answer that everybody says. It’s different, well, it depends. And it’s true because again, it depends on kind of what their status is. Are they a really critical patient? Well, hopefully if they’re a really critical patient we’re not sending them home to you and just saying, good luck, have fun. If they’re a really critical patient, we’re keeping them until they’re not critical anymore.
[00:37:20] >> Molly Jacobson: Right.
[00:37:21] >> Tasha Mcnerney: But yeah, inhalant anesthetic will linger around in the system. Um, it also depends on how cold they got during surgery, ’cause we know that if they get too hypothermic during the procedure, that’s gonna take longer for the anesthetics gonna work their way outta the body because the metabolism is just gonna be slow. So that plays into it as well. But because some of the opioids and the regional anesthesia and the inhalant anesthesia is kind of all swarming around in there, it does take a couple hours.
I usually tell people plan on it being 12 to 24 hours before their dog is kind of out of that anesthetic fog. And a lot of times we’re also sending them home with things like Tylenol with Codeine. We’re sending them home with Gabapentin. So these things, again, will act on, you know, ’cause gabapentin is going to function kind of similarly to like an SSRI, and so does a drug like Trazodone. So you’re gonna see some sedation.
So a lot of these drugs that you’re gonna go home with postoperatively to keep them kind of calm and quiet are going to cause some sedation in themselves. So I always tell people, you wanna just be really careful if your house has stairs or slippery floors. You can sometimes wanna sling your animals, leash walks only, and we usually, after surgery, don’t want ’em just kind of running around in the backyard by themselves, especially if they’re under the influence of opioids like Codeine, ’cause they could slip and fall and hurt themselves.
So we do wanna make sure that the owners are staying vigilant on the patients postoperatively.
[00:38:55] >> Molly Jacobson: So that’s interesting because I, I’ve always thought like, oh, don’t let them run around was about like pulling stitches, but it’s also because they’re almost certainly still sedated a bit from the anesthesia that’s lingering. Also, you’re giving these postoperative pain meds that have sedating qualities and so it’s like, don’t operate heavy machinery on this drug.
[00:39:15] >> Tasha Mcnerney: Yep. 100%.
[00:39:16] >> Molly Jacobson: Don’t operate your dog. Okay.
[00:39:17] >> Tasha Mcnerney: And especially if an animal has had orthopedic surgery, like one of the things I usually ask the owners is, where does this animal usually sleep at night? Because if the animal usually goes upstairs and sleeps with you in bed or at the bottom of your bed, there has to be a way that we can get that animal upstairs. So are you prepared to carry that animal upstairs? Because they should not be doing stairs by themselves. So we have to have a whole talk about the sleeping arrangements.
How does the animal go outside to go to the bathroom? Does he have to go down five or six stairs off the deck to get to the bathroom? If so, he’s gonna need help doing that. So there’s a lot of kind of owner conversation that we have to have to make sure that while he’s under the influence of opioids or the anesthesia’s lingering, he’s not gonna injure himself further.
[00:40:01] >> Molly Jacobson: Right, so that’s an important thing. I think a lot of people are surprised there’s so much work to do after surgery, but there really is at home, like there’s a lot of post-operative care that we should think about ahead of time and plan for. You know, there’s something that I’ve always wondered about why can’t dogs have breakfast before surgery, before anesthesia? What is that about?
[00:40:23] >> Tasha Mcnerney: Yeah. So unless they’re like a really tiny patient, so like a, you know, those little teacup Yorkies, those really tiny, like two and a half pound patients, those ones, we are a little more forgiving. We maybe don’t want them to be fasted too long cause their blood sugar can drop when they’re really tiny.
But for the most part, the reason that we want them to be fasted before they undergo anesthesia is because we don’t want to have them regurgitate or vomit while they’re under anesthesia or while they’re under the influence of drugs, and then we can have some regurgitant or vomiting that will come back down into the lungs.
[00:40:58] >> Molly Jacobson: Oh.
[00:40:58] >> Tasha Mcnerney: And we have seen this before and it can cause what’s known as aspiration pneumonia. These patients usually will get a pretty severe pneumonia. They may even have to be hospitalized for the pneumonia and be on some heavy duty antibiotic drugs. And we wanna prevent that from happening. And one of the ways we can prevent that from happening is making sure that they don’t have a lot of stomach contents in when we give them drugs like opioids, like Alpha-2 agonists, like all of the anesthetic drugs that we use, which tend to cause nausea and vomiting.
[00:41:28] >> Molly Jacobson: Okay. I see. So it’s really just about like, you know these, this, a common side effect of these anesthetics and opioids and sedatives could be nausea. So you don’t want them to throw up the contents of their breakfast. Because I know a lot of you, I certainly do, I feel so worried about, about my dog before-
[00:41:46] >> Tasha Mcnerney: Yeah.
[00:41:47] >> Molly Jacobson: -she goes into surgery. I wanna give her, you know, a nice breakfast before she has to go spend a horrible day at the vet. So, but don’t do it, you’re saying.
[00:41:55] >> Tasha Mcnerney: Don’t do it. Yeah, I know we’re tempted, but don’t do it because, yeah. Really the risk of aspiration pneumonia is much greater to them than maybe the disappointment of not having that breakfast that morning.
[00:42:10] >> Molly Jacobson: Okay. Yeah, it’s very difficult, but I can understand why. So if your dog has trouble with anesthesia, but then has to undergo it again for some other surgery or procedure, what does the vet need to take into account or what is the, you as a tech, have to take into account as a VTS?
[00:42:29] >> Tasha Mcnerney: Yeah, so I have this happen quite a lot, uh, where somebody will say, my pet had a bad reaction to anesthesia before, so I’m hesitant to undergo anesthesia again. And what you wanna do is, me as a technician specializing in anesthesia, I wanna make sure I really review that record. And make sure that I wanna say, where did it go wrong? Did it go wrong because of a certain drug? Did it go wrong because of a certain monitoring parameter that, you know, got messed up?
Maybe we could have helped the blood pressure but we ignored it, I’m not really sure, so I need to get all the facts before we just kind of make a judgment and do or not do. But I would say the best thing that we can do if the patient needs to undergo anesthesia again and has had an adverse reaction in the past, many, many anesthesiologists at university hospitals will offer drug consults or anesthesia protocol consults to local veterinarians for free.
[00:43:25] >> Molly Jacobson: Oh.
[00:43:25] >> Tasha Mcnerney: So if your veterinarian needs help coming up with a protocol or discussing an anesthetic protocol or anesthetic event, I would tell any veterinarian to reach out to the local teaching hospital, because many of these anesthesiologists will offer consults and help walk you through a case if it’s a difficult case.
Conversely, if your patient has had an anesthetic negative reaction in the past, if you’re an owner and you have the means, go to a university or to a specialty practice that has a boarded anesthesiologist on staff, that is ultimately gonna be the safest route to go.
[00:43:59] >> Molly Jacobson: So that the person who’s actually overseeing that case directly is a board certified anesthesiologist.
[00:44:06] >> Tasha Mcnerney: Correct.
[00:44:07] >> Molly Jacobson: That makes a lot of sense. What kinds of surgeries, because our listeners are people whose dogs have cancer, unfortunately, what kinds of surgeries or procedures commonly happen in cancer that might require anesthesia?
[00:44:25] >> Tasha Mcnerney: Yeah, so I mean, sometimes for some injections of some chemotherapies, we do need them to be under a little bit of light sedation, right, so we don’t happen to get anything extravascularly. But surgical wise or surgical anesthesia, the most common ones we see are ones where we have abdominal tumors where we might need to go in and remove a tumor, or we have osteopathic tumors where we might need to remove a limb. Or especially since I, um, worked with a boarded dentist for a little bit, we have kind of tumors of the mouth.
Maybe you have something on the tongue or something associated with a tooth or the jaw, and then we have to go in and do something like a maxillectomy or a mandibulectomy where we’re taking a section of the jaw that contains that tumor out. Kind of taking it out of the body, getting the best margins that we can, sending them out for biopsy, and then kind of making sure, again, we keep that patient as pain free as possible so they can go on to kinda live the best quality of life they can.
[00:45:26] >> Molly Jacobson: Not everybody gets radiation, obviously, but radiation also requires some anesthesia, doesn’t it?
[00:45:32] >> Tasha Mcnerney: Yes. I would say that it’s less common again, only because a lot of our clients seem to just not go for that option.
[00:45:41] >> Molly Jacobson: Yeah.
[00:45:41] >> Tasha Mcnerney: And I think that’s part of it is because of, you know, the cost when we look at the like cost to outcome. You know, like looking at the cost benefit, I guess we should say. I don’t have a lot of people that tend to go that route, but certainly yes, we will put them under anesthesia for interventional radiation as well.
[00:46:00] >> Molly Jacobson: What about imaging? Is there any kind of testing or imaging that needs anesthesia?
[00:46:06] >> Tasha Mcnerney: Yes. Now, sometimes we can do radiographs, so just basic radiographs, kind of under that twilight anesthesia or sedation, as I talked about before. But say we are going to go in and we have an abdominal tumor. A lot of times we wanna make sure that that abdominal tumor isn’t kind of intertwined with any of the big vasculature that we would really care about, or if they have a thoracic tumor.
So before we undergo surgery with them, they often will have a CT or an MRI just so we can kind of plan out how invasive the tumor is, where we’re gonna go, what we need as far as the surgery goes. And so yes, CT and MRI do require general anesthesia. Again, because if you go and get an MRI, I can say to you, all right, this is gonna be 10 minutes, I just need you to lay as flat as possible, listen to this music. We can’t do that with a dog.
[00:46:57] >> Molly Jacobson: Right. No. That’s just not gonna happen.
[00:46:59] >> Tasha Mcnerney: No.
[00:47:00] >> Molly Jacobson: So before we wrap up, I always like to ask, what is your like highest and best advice, with all of your hard-earned wisdom and your incredible training, what is your highest and best advice for listeners whose dogs have cancer, about anesthesia or any other thing that comes to mind?
[00:47:21] >> Tasha Mcnerney: Yeah, because my specialty is anesthesia and pain management, I would say listeners, just like everything else in medicine, you have to be the advocate, right? You have to be your own advocate in healthcare, and you have to be their advocate when we’re talking about taking them to the veterinarian. And if you feel like your pet is in pain, be that advocate.
I don’t care if you’re a pain in the ass, like, you know, be a pain in the ass for the sake of your patient. I certainly am when it came to my dog. So be an advocate for your patient and if you feel like they’re in pain, trust that instinct and ask for pain control for them. And I say that because there are some places out there that still will make postoperative pain control an optional thing on the surgical estimate or the checklist.
And I want you guys to know that if we did an abdominal procedure on a human, it’s going to feel the same on your dog. So please, please, please be an advocate for pain control in your patients and your pets as well.
[00:48:22] >> Molly Jacobson: Well, thank you so much. This was amazing. There’s so much to know about anesthesia and I so appreciate you joining us to help us understand a little bit better, ’cause it’s kind of mysterious, right? For the layperson.
[00:48:35] >> Tasha Mcnerney: Yeah, it is kind of a mysterious thing, but again, very fascinating and very cool at the same time.
[00:48:41] >> Molly Jacobson: Yeah. Thank you so much for joining us today.
[00:48:44] >> Tasha Mcnerney: Yeah, thanks so much for having me.
[00:48:48] >> Molly Jacobson: And thank you, listener. It really is stressful when your dog needs to go under anesthesia. I know that’s one of the things I worry about the most as a dog mom. But rest assured, the trained technicians working with your dog can do a lot to make sure that everything goes smoothly. If you aren’t sure about the credentials and training of veterinary staff in your local area, your state, or your country, make sure you ask and get some peace of mind.
And for more information on surgery and anesthesia for dogs with cancer, visit our website at dogcancer.com and browse the articles or search previous episodes of Dog Cancer Answers. You can also visit us on YouTube and leave a comment with your anesthesia experience with your dog.
I’m Molly Jacobson, and from all of us here at Dog Podcast Network, I’d like to wish you and your dog a very warm Aloha.
[00:49:45] >> Announcer: Thank you for listening to Dog Cancer Answers. If you’d like to connect, please visit our website at dogcanceranswers.com or call our Listener Line at (808) 868-3200. And here’s a friendly reminder that you probably already know: this podcast is provided for informational and educational purposes only. It’s not meant to take the place of the advice you receive from your dog’s veterinarian.
Only veterinarians who examine your dog can give you veterinary advice or diagnose your dog’s medical condition. Your reliance on the information you hear on this podcast is solely at your own risk. If your dog has a specific health problem, contact your veterinarian. Also, please keep in mind that veterinary information can change rapidly, therefore, some information may be out of date.
Dog Cancer Answers is a presentation of Maui Media in association with Dog Podcast Network.
Hosted By
SUBSCRIBE ON YOUR FAVORITE PLATFORM
Topics
Editor's Picks
CATEGORY